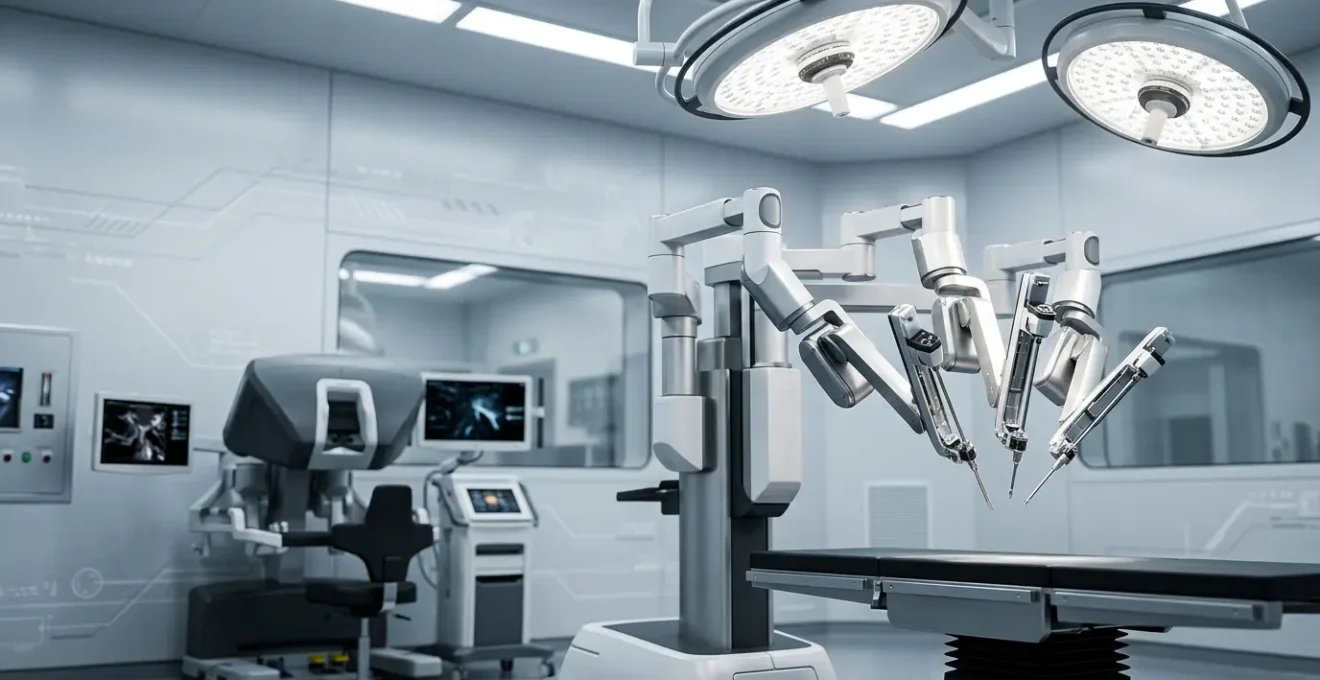
The key to superior tumor margins isn’t just the robot’s steady hand; it’s the adoption of a complete, data-driven surgical operating model that the technology enables.
- Achieving negative margins consistently relies on a system of scalable surgeon proficiency, optimized workflows, and the integration of real-time data.
- The financial viability of a robotics program is directly linked to high case volume, which in turn fuels the very expertise required for complex oncological procedures.
Recommendation: As a leader, shift your focus from evaluating the robot as a tool to implementing it as the core of a new, more effective, and marketable system for oncological care.
As leaders in surgical innovation, we are constantly pursuing the ultimate goal in cancer surgery: the complete removal of a tumor with clean, negative margins. For decades, the conversation has centered on the surgeon’s skill, tactile feedback, and visual acuity. The introduction of robotic surgery is often simplified to the idea of a « more precise instrument » or « better 3D vision. » While true, this perspective misses the profound, systemic revolution unfolding in our operating rooms.
The real genius of modern robotics in achieving superior resection margins lies far beyond mechanical stability. It’s about a fundamental paradigm shift. We are moving from a practice reliant on individual artistry to a data-driven, systems-based approach to surgery. The robot is not merely a better scalpel; it is the central hub of a new surgical workflow that integrates imaging, analytics, and team-wide proficiency into a cohesive, scalable, and economically powerful model. This isn’t just an upgrade; it’s a re-architecting of how we approach oncological resection.
This article moves beyond the surface-level benefits to provide a strategic overview for department heads and innovators. We will explore how the true value of robotics is unlocked not by the machine alone, but by a holistic strategy encompassing economic models, rapid training, environmental design, and marketing. We will deconstruct the components that transform a multi-million-dollar capital investment into a center of excellence defined by its superior clinical outcomes—specifically, its ability to consistently deliver negative surgical margins.
To navigate this strategic shift, this guide breaks down the critical operational and design questions you need to answer. The following sections will provide a comprehensive framework for building and optimizing a world-class robotic surgery program, focusing on how each component contributes to the ultimate clinical goal of superior oncological outcomes.
Summary: A Strategic Guide to Robotic Surgery and Tumor Margin Excellence
- Why the ROI of Surgical Robots Depends on High Case Volume Utilization?
- How to Certify Surgeons on Robotic Consoles in Under 3 Months?
- Single-Port vs. Multi-Port Systems: Which Is Better for ENT Procedures?
- The Network Bandwidth Issue That Causes Lag in Telesurgery
- How to Market Your Hospital’s Robotic Program to Attract Local Patients?
- Why Ceiling-Mounted Angiography Systems Save Vital Floor Space in Hybrid ORs?
- How to Set Up a Low-Cost Clinical Simulation Lab for Nursing Staff?
- How to Design a Hybrid Operating Room That Supports Both Cardiac and Neuro Surgery?
Why the ROI of Surgical Robots Depends on High Case Volume Utilization?
The multi-million-dollar price tag of a surgical robot is the first hurdle for any hospital innovator. Justifying this investment requires a clear-eyed look at the economic engine of a robotics program: high case volume. The return on investment isn’t generated by simply owning the technology, but by maximizing its utilization. High volume creates an economic viability loop where the cost per procedure decreases, making the program financially sustainable. More importantly, it is the bedrock of clinical excellence. A busy robotic OR is an experienced robotic OR.
This constant use fosters a level of team cohesion and surgeon proficiency that is impossible to achieve with sporadic cases. The entire team—from the console surgeon to the bedside assistant and circulating nurse—develops an intuitive, efficient workflow. This operational tempo directly translates into better clinical outcomes, including the consistent achievement of negative margins. The data is compelling; one extensive analysis of the UK’s NHS found that implementing robotic surgery led to a 50% reduction in total length of stay and a significant decrease in post-operative visits, demonstrating massive efficiency gains.
Furthermore, this efficiency drives productivity across the hospital. A separate study confirmed that the adoption of robotic techniques can increase a hospital’s total surgical production by between 21% and 26%, coupled with a 29% improvement in labor productivity. This isn’t just about doing more cases; it’s about optimizing the entire surgical service line. For a program director, the mandate is clear: build a strategy that feeds the robot. This involves careful procedure selection, surgeon scheduling, and marketing efforts designed to ensure the console never sits idle, transforming a capital expense into a high-yield asset for clinical and financial performance.
How to Certify Surgeons on Robotic Consoles in Under 3 Months?
To achieve the high case volume necessary for ROI, we need a pipeline of proficient surgeons. The traditional apprenticeship model is too slow and inconsistent for the demands of a modern robotics program. The challenge, then, is to accelerate the learning curve without compromising safety or quality. The answer lies in establishing a structured, data-driven pathway to certification that can create highly competent console surgeons in a fraction of the time. This is the key to achieving scalable proficiency across an entire department.
The enthusiasm for adoption is already present. With over 78% of US surgeons expressing interest in adopting robotic techniques, the demand for effective training is critical. An accelerated certification program moves beyond simple case observation. It leverages technology to build and measure skill. Proficiency-based training on simulators becomes the first gate, using objective metrics for economy of motion, clutching, and tissue handling to ensure a surgeon has the core psychomotor skills before ever approaching a patient.
The next layer involves patient-specific virtual rehearsal. Using 3D models generated from a patient’s own MRI or CT scans, a surgeon can practice the most critical parts of a complex tumor resection beforehand, identifying potential challenges in a zero-risk environment. This data-driven preparation is then combined with a tiered mentorship program and team-based certification that includes the entire OR staff. By the time a surgeon performs their first cases, they can be guided in real-time via tele-proctoring, ensuring expert oversight. This systematic approach transforms surgeon training from a subjective art into a reproducible science, enabling a program to scale its talent pool rapidly and safely.
Action Plan: Rapid Robotic Surgery Certification
- Implement Proficiency-Based Simulation: Use simulator metrics for economy of motion and tissue handling to establish objective skill benchmarks before clinical work.
- Utilize Patient-Specific Virtual Rehearsal: Create 3D models from patient CT/MRI scans for pre-operative practice on critical procedure steps.
- Establish a Tiered Mentorship Program: Structure a gradual increase in task complexity under the guidance of an experienced proctor.
- Deploy Team Certification Models: Ensure the entire team, including bedside assistants and nurses, is certified together to optimize workflow and communication.
- Use Tele-proctoring for Initial Cases: Provide real-time remote guidance from expert surgeons during the first set of independent procedures.
Single-Port vs. Multi-Port Systems: Which Is Better for ENT Procedures?
Once a program is established, technical specialization becomes the next frontier of optimization. For disciplines like Ear, Nose, and Throat (ENT) surgery, the choice between a single-port (SP) and a multi-port robotic system is a critical strategic decision. This isn’t just about the number of incisions; it’s about which system architecture best facilitates access and maneuverability within the constrained anatomy of the head and neck. Multi-port systems offer robust triangulation, a familiar paradigm for laparoscopy, but can be challenging to position without external collisions in ENT cases.
The emergence of SP systems, however, represents a significant evolution in surgical workflow integration for this specialty. By consolidating instruments and the camera into a single arm, the SP robot can access deep, narrow spaces through a single entry point, like the oral cavity. This approach minimizes the external footprint and maximizes internal reach, which is paramount for procedures like Transoral Robotic Surgery (TORS).
As the instrumentation detail above suggests, the engineering focus is on maximizing articulation in confined spaces. The clinical results for TORS in achieving negative margins are profound. A detailed analysis of TORS procedures for complex parapharyngeal space tumors showed that surgeons achieved complete tumor resection with an intact capsule in 93% of patients. Margin involvement was exceptionally rare, occurring in only two cases and was attributed to tumor capsule rupture. This demonstrates that for specific applications like ENT, the SP system’s architecture is not just a matter of convenience; it is a direct enabler of superior oncological outcomes, allowing surgeons to perform more complete resections in areas previously deemed difficult to access.
The Network Bandwidth Issue That Causes Lag in Telesurgery
As we push the boundaries of robotic surgery, the horizon is dominated by telesurgery—the ability to operate on a patient from miles away. This vision promises to democratize surgical expertise, but it hinges on one non-negotiable factor: near-zero latency. Lag, or the delay between the surgeon’s hand movements and the robot’s response, is the single greatest threat to the safety and efficacy of remote procedures. It breaks the intuitive connection between surgeon and instrument, transforming a precise tool into an unpredictable one. This is the ultimate threat to data-driven resection, as it corrupts the integrity of the data stream itself.
The acceptable margin for error is incredibly slim. Scientific consensus confirms that for a surgeon to maintain precision and avoid catastrophic errors, latency must remain below a 200-millisecond threshold. Every millisecond above this introduces a disconnect that can lead to inadvertent tissue damage, failed dissections, and compromised tumor margins. This is not just a technical specification; it is a fundamental patient safety requirement. The challenge for innovators is building a network infrastructure—combining fiber optics, 5G, and satellite backups—that can guarantee this level of performance over hundreds or even thousands of miles.
The feasibility of this is no longer theoretical. We are witnessing the dawn of intercontinental surgery, proving that this barrier can be overcome with visionary engineering and robust network architecture.
Case Study: The Shanghai-Kuwait Intercontinental Telesurgery Achievement
In a landmark achievement, surgeons in Shanghai successfully performed a robotic-assisted radical prostatectomy on a patient in Kuwait, over 4,500 miles away. The procedure was made possible by a dedicated network infrastructure that maintained an average round-trip latency of just 181.4 milliseconds, well within the safe threshold. The result was a clinical masterpiece: the patient achieved negative surgical margins (pT2Nx), was continent within a week, and had an undetectable PSA level at seven weeks post-op. This case proves that with the right network design, distance is no longer a barrier to expert surgical care.
How to Market Your Hospital’s Robotic Program to Attract Local Patients?
Developing a world-class robotic surgery program with outstanding clinical outcomes is only half the battle. To fuel the high case volume needed for ROI and continued excellence, you must effectively communicate your program’s value to the community. Marketing a robotics program is a nuanced task. It’s not about advertising a machine; it’s about building trust and showcasing superior results in a way that resonates with patients and referring physicians. The core of this strategy is translating complex clinical data, like negative margin rates, into a compelling message of hope and peace of mind.
A successful marketing framework operates on two parallel tracks. For referring physicians, the focus should be on clinical data, peer-reviewed publications, and program statistics that demonstrate outcomes superior to national averages. This builds clinical credibility. For patients, the messaging must be centered on benefits. Instead of « high negative margin rates, » use patient-centric language like « the peace of mind that comes from a more complete cancer removal. » Patient testimonials are incredibly powerful, especially when they focus not just on the fast recovery, but on the long-term oncological success and the quality of their follow-up care.
Crucially, the marketing should highlight the entire team’s expertise, not just the robot. Feature your specially trained nurses, assistants, and the continuous education programs you have in place. This communicates a culture of excellence and safety that goes beyond the hardware. The goal is to build a brand reputation as the definitive local leader in minimally invasive cancer care, where technology is wielded by a deeply experienced and dedicated team. This approach attracts patients, satisfies referring physicians, and ultimately drives the volume that sustains the entire program, closing the economic viability loop.
Why Ceiling-Mounted Angiography Systems Save Vital Floor Space in Hybrid ORs?
As we design the operating rooms of the future, our focus expands from the surgical table to the entire environment. In a hybrid operating room—a space designed for both open and minimally invasive procedures, often combined with intraoperative imaging—floor space is the most valuable commodity. Traditional floor-based equipment, from C-arms to monitoring carts, creates a cluttered, hazardous environment. This is where ceiling-mounted systems represent a revolutionary leap in OR design and system-level precision.
By suspending heavy imaging equipment like angiography systems from ceiling-mounted booms, we reclaim the entire floor. This has immediate and profound benefits for the surgical workflow. As one leading publication notes, « A clutter-free floor reduces trip hazards, improves team ergonomics and movement, and allows for faster emergency response, particularly during complex procedures involving large teams. » The ability for a perfusionist, anesthesiologist, or nurse to move freely and quickly around the patient without navigating a maze of cables and equipment is a massive enhancement to patient safety and team efficiency.
This design philosophy, beautifully illustrated in the image of a modern hybrid OR, is about creating a flexible, multi-purpose space. The ceiling-mounted boom can position the imaging system precisely where it’s needed for a cardiac intervention, then retract it completely out of the way to create an open field for a neurosurgical procedure or to bring in a surgical robot. This flexibility allows one room to serve multiple high-revenue service lines, dramatically increasing its utilization and ROI. For the program director, championing ceiling-mounted design is not an aesthetic choice; it is a strategic decision to build a safer, more efficient, and more versatile surgical environment.
How to Set Up a Low-Cost Clinical Simulation Lab for Nursing Staff?
While the focus of robotic training is often on the console surgeon, the proficiency of the entire team is just as critical to a successful outcome. The bedside assistants and circulating nurses are the surgeon’s hands and eyes in the sterile field. Their ability to perform instrument exchanges, troubleshoot faults, and manage the OR flow can make or break a complex case. Delays caused by an unprepared team are not just frustrating; they are astronomically expensive. The financial impact of a delayed or canceled robotic case can exceed $2,000 per minute.
Investing in a high-fidelity robotic simulator for surgeons is a major capital expense, but building a culture of scalable proficiency for the nursing and support staff doesn’t have to be. A low-cost, high-impact clinical simulation lab can be established using readily available resources. The key is to focus on the specific, repeatable tasks that are critical during a robotic procedure. This doesn’t require a full-fledged robot.
A dedicated « dry lab » can be set up in a conference room or unused clinical space. It can be equipped with decommissioned instrument arms (often available from the manufacturer), training models, and video screens to simulate the OR environment. Here, nursing staff can practice docking the robot, changing instruments, managing drapes, and running through emergency undocking procedures in a low-stress environment. Using checklists and timed drills, you can build muscle memory and create a standardized, team-wide response to common and critical situations. This small, targeted investment in staff training yields enormous returns by minimizing downtime, reducing errors, and fostering a culture of preparedness that directly supports the surgeon’s ability to focus on the delicate task of tumor resection.
Key Takeaways
- The success of a robotic surgery program hinges on treating the robot as the center of a new operating system, not just a standalone tool.
- High case volume is the engine of both financial ROI and clinical proficiency, creating a feedback loop of excellence.
- Systemic design, from rapid surgeon certification and team simulation to the physical layout of the OR, directly impacts clinical outcomes like negative margin rates.
How to Design a Hybrid Operating Room That Supports Both Cardiac and Neuro Surgery?
The ultimate expression of surgical systems integration is the multi-disciplinary hybrid operating room. Designing a single space that can flawlessly support the divergent needs of cardiac and neurosurgery is the pinnacle of hospital innovation. This is no longer just about accommodating a surgical robot; it’s about creating a unified data and equipment ecosystem. As a visionary from the Healthcare Architecture Journal puts it, the core mandate must be to « Design for ‘Data Fusion’… Plan the room’s digital architecture to integrate all data streams—robotics, imaging, EMR, patient monitors, pathology—into a central hub. »
This challenge goes far beyond just having enough space. The workflows and equipment priorities for these two disciplines are fundamentally different. A cardiac procedure requires a standing team and prioritizes space for perfusion equipment and heart-lung machines. A neurosurgical procedure often involves a seated surgeon, relies on intraoperative MRI capability, and demands dedicated zones for neuromonitoring stacks and high-powered microscopes. A successful design must accommodate both scenarios without compromise.
This requires a modular approach using ceiling-mounted booms, adaptable equipment layouts, and strategically placed power and data ports. The goal is to create a « plug-and-play » environment where the room can be reconfigured in minutes. The following table highlights the distinct requirements that must be harmonized in a truly versatile hybrid OR design.
| Design Element | Cardiac Surgery Requirements | Neurosurgery Requirements |
|---|---|---|
| Team Position | Standing configuration | Seated configuration |
| Equipment Zones | Perfusion equipment priority | Neuromonitoring stacks priority |
| Imaging Integration | Cardiac catheterization focus | Intraoperative MRI capability |
| Power/Data Ports | Heart-lung machine connections | Microscope and navigation systems |
| Robot Footprint | Cardiac-specific platforms | Cranial access requirements |
As this comparative analysis of design elements shows, the complexity is immense. Designing a successful multi-disciplinary hybrid OR is a masterclass in strategic planning. It requires close collaboration between surgeons, architects, and IT specialists to build a future-proof platform that not only supports today’s technology but is ready for the integrated, data-fused procedures of tomorrow.
As leaders, embracing this systemic view of robotic surgery is our primary responsibility. By focusing on the integration of people, processes, and technology, we can build programs that not only justify their investment but also set a new standard in cancer care. The path to consistently achieving negative tumor margins lies in this holistic, data-driven, and visionary approach. Now is the time to lead this transformation in your institution.