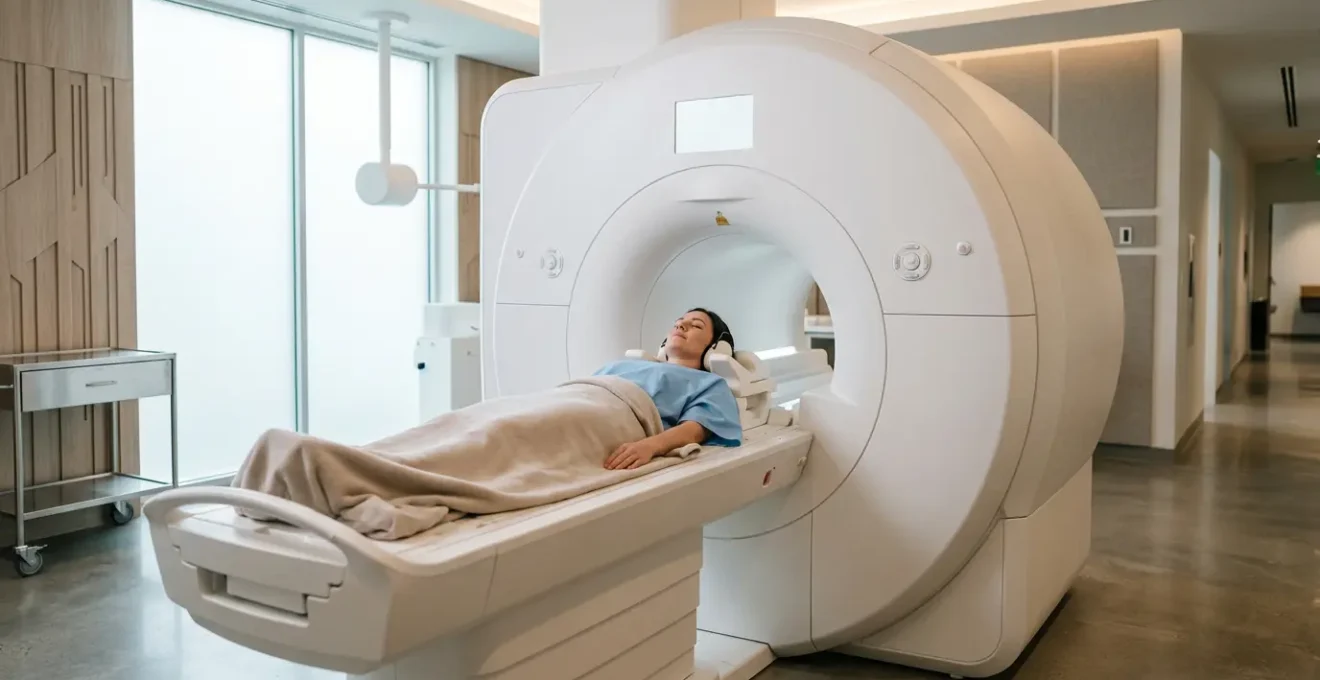
Achieving a 30% reduction in MRI scan times for anxious patients is not about a single machine, but a deliberate operational symbiosis of hardware, software, and workflow.
- Hardware like 70cm bores and advanced noise reduction technology directly mitigates the primary causes of patient-induced variability and motion artifacts.
- Proactive asset management through models like MES and vigilant helium monitoring prevents costly downtime and ensures ongoing technological relevance.
Recommendation: Shift from piecemeal upgrades to a holistic strategy that treats patient experience as a direct driver of operational efficiency and diagnostic quality.
Every MRI technologist and neurologist knows the feeling: the final, critical sequence of a 45-minute scan is underway, and the patient moves. The artifact renders the images non-diagnostic, and the entire process must be repeated. This scenario, often rooted in patient anxiety or claustrophobia, is more than just a scheduling inconvenience; it’s a significant drain on departmental efficiency, a source of patient distress, and a direct threat to diagnostic confidence. For managers, it represents lost revenue and reduced throughput. For clinicians, it means delayed diagnoses.
The common responses are often tactical rather than strategic: use a mild sedative, offer a blindfold, or simply invest in the widest bore magnet available and hope for the best. While these measures have their place, they treat the symptoms, not the underlying operational challenge. The true source of inefficiency is often patient-induced variability—the unpredictable element of human fear and discomfort that sabotages carefully planned schedules and high-field-strength magnets.
But what if the solution wasn’t just about making the patient more comfortable, but about re-engineering the entire scanning environment to systematically reduce this variability? This article takes a different approach. We will explore how a strategic, multi-layered integration of advanced MRI technologies transforms patient comfort from a ‘soft’ benefit into a hard metric for operational performance. We will move beyond the single specification sheet and look at how magnet design, acoustic noise reduction, field strength trade-offs, and even service models create an operational symbiosis that directly addresses the root causes of patient-induced delays, ultimately leading to faster, more reliable, and more profitable scanning.
This guide provides a framework for managers and neurologists to evaluate and implement technology not just for its imaging capability, but for its power to create a predictable, efficient, and patient-centered service. We will explore the specific hardware, software, and protocols that form the foundation of a modern, high-throughput imaging center.
Summary: A Manager’s Guide to MRI Efficiency and Patient Experience
- Why 70cm Bore Magnets Are Essential for Bariatric Patient Accessibility?
- How to Reduce MRI Acoustic Noise to Conversation Levels for Pediatric Patients?
- 1.5T vs. 3T MRI: Which Field Strength Provides Better Musculoskeletal Detail?
- The Ferromagnetic Detection Oversight That Leads to Projectile Accidents
- How to Monitor Helium Levels to Prevent Costly Quench Events?
- Why Iterative Reconstruction Techniques Lower Patient Dose by Up to 50%?
- Why Managed Equipment Services (MES) Are Replacing Capital Purchases?
- How to Choose Medical CT Scanner Technology That Balances Dose and Image Quality?
Why 70cm Bore Magnets Are Essential for Bariatric Patient Accessibility?
The physical dimensions of an MRI scanner represent the first and most significant barrier to care for a growing patient population. For bariatric patients and those with severe claustrophobia, a standard 60cm bore is often a non-starter, leading to cancelled appointments or the need for complex and costly patient transfers. A 70cm wide-bore magnet is not a luxury; it’s a foundational piece of equipment for ensuring equitable access and maintaining operational flow. The immediate benefit is the ability to accommodate a wider range of body habitus. Modern wide bore MRI machines can accommodate patients weighing up to 550-660 pounds, a substantial increase from the 400-pound limit of many traditional systems.
This expanded capacity directly translates to fewer patient rejections and a wider referral base. However, the strategic impact goes deeper. For facilities without this capability, the logistical burden can be immense, requiring carefully coordinated transfers to other centers. The operational complexity and cost of these transfers are significant, often reserved for only the most urgent clinical needs.
As the visual comparison shows, the increased diameter does more than just fit larger patients; it fundamentally changes the patient’s perception of the space. This reduction in physical confinement is a powerful tool against claustrophobia, decreasing the likelihood of panic-induced motion or early termination of the exam. By investing in a 70cm bore, a facility is not just buying a larger machine; it is investing in schedule predictability and minimizing the high downstream costs associated with managing patient transfers and failed scans.
How to Reduce MRI Acoustic Noise to Conversation Levels for Pediatric Patients?
After confinement, the single greatest source of patient anxiety during an MRI is the intense acoustic noise, which can reach levels comparable to a rock concert. For pediatric patients, this noise can be terrifying, making cooperation nearly impossible without sedation. For anxious adults, it’s a major contributor to stress that leads to motion artifacts. Addressing this requires moving beyond standard earplugs and headphones to implementing sequences with fundamentally quieter designs. Modern noise reduction technologies represent a paradigm shift in patient experience management.
Leading manufacturers have developed innovative solutions that tackle noise at the source—the rapid switching of gradient coils. For instance, some platforms offer a comprehensive software package that can perform complete neuro and orthopedic exams at near-ambient noise levels. Clinical data from these systems is compelling; technologies like Quiet Suite have been shown to reduce MRI acoustic noise by up to 97%. This transforms the scanning environment from one of intimidation to one of relative calm, drastically improving the experience for sensitive patients. As Dr. Noriko Aida of Kanagawa Children’s Med Center in Japan notes:
The quiet sequences are gentle for children and have been very useful in imaging pediatric patients. They provide a more comfortable scanning environment without compromising image quality.
– Dr. Noriko Aida, Kanagawa Children’s Med Center, Japan
For facility managers, the choice of technology involves evaluating a competitive landscape of solutions, each with distinct features. Understanding these differences is key to making an informed investment that aligns with the specific needs of your patient population, particularly if it includes a high volume of pediatric or neuro-imaging cases.
| Technology | Manufacturer | Noise Reduction | Key Features |
|---|---|---|---|
| Silent Scan | GE Healthcare | Reduces to 69 dB | Eliminates noise at source |
| ComforTone | Philips | Up to 80% reduction | Maintains scan time and image quality |
| Quiet Suite | Siemens | Up to 97% reduction | Complete neuro and orthopedic exams |
1.5T vs. 3T MRI: Which Field Strength Provides Better Musculoskeletal Detail?
The debate between 1.5 Tesla (T) and 3T field strengths is often oversimplified to « 3T is better. » While a 3T magnet offers a fundamentally higher signal-to-noise ratio (SNR), which can be leveraged for higher resolution or faster scan times, it is not universally superior for all applications, especially in musculoskeletal (MSK) imaging. The optimal choice depends on a nuanced understanding of the trade-offs between signal, artifacts, and clinical objectives.
A 3T system’s primary advantage is its ability to acquire images with finer detail in a shorter amount of time. This is invaluable for advanced applications like cartilage mapping or high-resolution nerve imaging. However, this increased field strength also amplifies certain challenges. Susceptibility artifacts, caused by the presence of metal (e.g., post-surgical implants), are significantly more pronounced at 3T, potentially obscuring nearby anatomy. Furthermore, dielectric effects can cause signal loss and non-uniformity in images of large body parts, like the abdomen or pelvis, an effect that is less prominent at 1.5T.
For many routine MSK applications—such as evaluating a knee for a meniscal tear or a shoulder for a rotator cuff injury—a modern 1.5T scanner equipped with advanced, high-channel coils and sophisticated reconstruction software often represents the ideal balance. These systems provide excellent diagnostic quality with fewer artifacts, particularly in post-operative patients. The decision should not be based on field strength alone, but on a « Signal-to-Noise-to-Speed Ratio » (SNSR) analysis that considers the specific clinical questions, patient population (e.g., prevalence of implants), and the overall capabilities of the scanner, including its coils and software. For a general MSK-focused practice, a high-performance 1.5T can be the more robust and versatile workhorse.
The Ferromagnetic Detection Oversight That Leads to Projectile Accidents
The MRI suite is one of the most hazardous environments in a hospital, yet safety protocols can become dangerously routine. The very factors that drive the need for faster scans—high patient volume and anxiety—can also create a high-stress environment where safety checks are rushed and oversights occur. Data shows that a significant percentage of scans fail due to patient distress; clinical studies indicate that between 0.5% and 14.5% of MRI exams fail due to claustrophobia, creating pressure on staff to expedite procedures. This pressure can lead to catastrophic oversights in ferromagnetic safety.
A projectile accident, where a ferromagnetic object is pulled into the magnet bore, is an entirely preventable event rooted in procedural failure. Relying solely on patient questionnaires and staff vigilance is insufficient. A robust safety program requires an engineered, multi-layered approach that assumes human error will occur. This involves creating a system of physical barriers, detection technologies, and formal protocols that make it difficult for mistakes to happen. The concept of MRI Safety Zones (I-IV) is the backbone of this system, with Zone IV being the scanner room itself.
The workflow illustrated above, with clear demarcation of zones, is a visual representation of a system designed to prevent error. Entry into Zone IV must be a hard-stopped, formal process. Implementing ferromagnetic detection systems (FMDS) at the entrance to this zone acts as a final, crucial checkpoint. However, technology alone is not enough; it must be integrated into a comprehensive safety culture that emphasizes training, reporting, and constant vigilance.
Action Plan: Key Components of a Projectile-Proof MRI Safety Protocol
- System Implementation: Install and mandate the use of ferromagnetic detection systems (FMDS) at all entry points to MRI Safety Zone IV.
- Procedural Formalization: Establish a « near miss » reporting system to analyze and learn from potential safety breaches before an accident occurs.
- Physical Environment Design: Use clear physical barriers and « red line » floor markings to visually and physically separate safe zones from the high-risk scanner room.
- Technologist Workflow: Require technologists to complete a formal, documented pre-scan safety checklist for every single patient, visitor, and staff member entering the room.
- Personal Item Management: Provide secure, locked storage for all personal items (keys, phones, wallets) well outside the restricted zones to eliminate accidental entry.
How to Monitor Helium Levels to Prevent Costly Quench Events?
While patient-facing technologies are critical, the operational stability of an MRI scanner depends on a component that is completely invisible: liquid helium. This cryogen keeps the superconducting magnet at its near-absolute zero operating temperature. The loss of this superconductivity, known as a « quench, » is an operational and financial disaster. It involves a rapid, violent boil-off of all liquid helium, rendering the magnet unusable until it can be cooled and refilled.
The financial implications are severe. The immediate cost for a helium refill alone is substantial, with some healthcare facility cost analyses citing figures between $20,000 and $50,000. This does not account for the lost revenue from scanner downtime, which can last for days or even weeks, nor the cost of emergency service calls and potential long-term damage to the magnet itself.
Preventing a quench hinges on proactive monitoring of the helium level and the health of the cryocooler system (or « coldhead ») that minimizes normal boil-off. A rising helium boil-off rate is a key early warning sign of impending coldhead failure. In legacy systems, this monitoring was often a manual, periodic check by technologists. However, modern scanners are increasingly equipped with automated, IoT-based monitoring systems. These sensors provide continuous, real-time data on helium levels and system temperature, sending automated alerts to facility managers and service engineers long before a critical situation develops. This shifts the maintenance posture from reactive to predictive, allowing for scheduled, low-cost service to prevent a catastrophic, high-cost failure.
Why Iterative Reconstruction Techniques Lower Patient Dose by Up to 50%?
While this article focuses on MRI, a truly efficient imaging department understands the interplay between modalities. In Computed Tomography (CT), the central challenge is not claustrophobia but radiation dose. The guiding principle of « As Low As Reasonably Achievable » (ALARA) forces a constant negotiation within the Dose-Image-Time Triangle. For decades, the primary method for reconstructing CT images was Filtered Back Projection (FBP). While fast, FBP has a major limitation: it amplifies image noise, especially at low radiation doses. To get a clean image, technologists often had to use a higher dose.
Iterative Reconstruction (IR) techniques fundamentally change this equation. Instead of a one-step mathematical process like FBP, IR is a cyclical process that starts with an assumed image, compares it to the raw scan data, and progressively refines the image to reduce the difference (or « error »). It uses sophisticated statistical models of the scanner’s physics and noise properties to intelligently distinguish between true anatomical signal and random noise. This « smart » denoising process is the key to its power.
By effectively removing noise from the image, IR allows technologists to use significantly lower radiation dose (mA) settings during the scan acquisition while still producing an image of equal or even superior diagnostic quality compared to a higher-dose FBP scan. This breakthrough is what enables the widely cited claim of dose reduction of up to 50% or more in many clinical applications. For managers and clinicians, adopting IR is a critical step in building a patient-centric and safety-conscious CT service, allowing for safer screening of pediatric patients and those requiring frequent follow-up scans without compromising diagnostic confidence.
Key Takeaways
- Patient-induced variability is a key bottleneck; technology that improves patient experience directly boosts throughput.
- A holistic approach combining wide-bore magnets, quiet sequences, and robust safety protocols creates an efficient and safe environment.
- Financial models like MES and proactive monitoring of critical systems like cryogen levels are as important as the imaging technology itself.
Why Managed Equipment Services (MES) Are Replacing Capital Purchases?
The traditional model for acquiring high-end imaging equipment has been a large, one-time capital expenditure (CapEx). This model forces facilities to be locked into a specific technology for its entire 7-10 year lifespan, even as innovation accelerates. In today’s rapidly evolving landscape, a scanner purchased just a few years ago can lack the critical software and hardware features—like advanced quiet sequences or iterative reconstruction—that are becoming the standard of care. This is where Managed Equipment Services (MES) are emerging as a more strategic financial and operational model.
An MES agreement shifts the paradigm from ownership to access. Instead of a massive upfront purchase, a facility pays a predictable, recurring operational expense (OpEx) to a vendor who provides, maintains, and upgrades the equipment over the contract term. This model offers several powerful advantages for a department manager. First, it eliminates the risk of technological obsolescence. Contracts typically include scheduled technology refreshes and upgrade paths, ensuring the facility always has access to modern capabilities. Second, it guarantees performance. MES contracts are built on service-level agreements (SLAs) with clear metrics for uptime (often 98% or higher) and penalties for non-performance, aligning the vendor’s incentives with the facility’s operational goals.
Case Study: Intermountain Medical Imaging’s MES Model
A real-world example of this model’s success is Intermountain Medical Imaging in Boise. Operating for over 20 years, they have leveraged a long-term service model to provide state-of-the-art technology like wide-bore MRI without the constraints of capital purchasing. Their approach demonstrates how an MES partnership allows a facility to focus on clinical care while the vendor manages the technology lifecycle, ensuring that they can consistently offer services that reduce patient anxiety and accommodate a broader patient demographic, ultimately improving detection rates for serious health conditions.
For managers negotiating an MES contract, key focus points should include defining clear vendor responsibilities for all maintenance and staff training, building in flexibility to adapt to changes in clinical demand, and ensuring the fee structure is truly predictable. This model transforms asset acquisition into proactive asset management, a crucial strategy for staying clinically relevant and financially sound.
How to Choose Medical CT Scanner Technology That Balances Dose and Image Quality?
Just as in MRI, the optimal choice in CT technology is not simply the one with the most detector rows or the fastest gantry speed. The ultimate goal is to find the perfect equilibrium in the Dose-Image-Time Triangle for each specific clinical task. A single, one-size-fits-all protocol is inefficient and can lead to either excessive radiation dose for simple cases or insufficient image quality for complex ones. A modern, efficient CT service is built on the principle of protocol optimization and the use of technology that facilitates it.
This involves creating a tiered system of scanning protocols tailored to different clinical needs. The ability to modulate dose based on the diagnostic question is a hallmark of an advanced CT program. For example, a low-dose lung cancer screening exam has a very different requirement than a detailed workup of a complex vascular anomaly. The former prioritizes detection with minimal dose, while the latter prioritizes maximum resolution, even if it requires more radiation. AI-powered reconstruction algorithms are now playing a pivotal role, enabling ultra-low-dose protocols that were previously unimaginable.
For managers and lead technologists, implementing a structured protocol tier system is a practical way to institutionalize the ALARA principle while ensuring clinical needs are met. This system ensures consistency, simplifies training, and provides a clear framework for dose management across the department.
The following table provides a conceptual model for such a tiered system, which can be adapted to any facility’s specific clinical demands and scanner capabilities.
| Protocol Tier | Clinical Application | Dose Strategy | Image Priority |
|---|---|---|---|
| Tier 1 | Screening exams | Ultra-low dose with AI reconstruction | Detection over detail |
| Tier 2 | Standard diagnostics | Balanced dose/quality | Clinical confidence |
| Tier 3 | Complex cases | Quality prioritized over dose | Maximum resolution |
To truly optimize your diagnostic imaging service, the next step is to conduct a full audit of your current technology stack and patient workflow against these modern benchmarks. Assess where patient-induced variability is costing you time and quality, and build a strategic roadmap for integrated technology adoption.
Frequently Asked Questions on MRI System Management
How do modern IoT sensors improve helium monitoring?
IoT-based sensors provide continuous real-time data, automated trend analysis, and instant alerts to facility managers and service providers, preventing emergency situations through predictive maintenance.
What is the significance of helium boil-off rate?
The boil-off rate serves as a key performance indicator of the magnet’s cryocooler system health. Sudden increases can predict hardware failures weeks in advance, allowing for scheduled maintenance.
How much downtime can a quench event cause?
Beyond the immediate helium replacement cost, facilities face lost revenue from scanner downtime, emergency service calls, and potential weeks of unavailability if magnet damage occurs.